Neonatal infection
| Neonatal infection | |
|---|---|
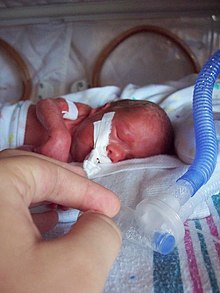 | |
| 26-week gestation, premature infant, weighing <990gm with ventilator | |
| Specialty | Infectious disease, Pediatrics |
Neonatal infections are infections of the neonate (newborn) acquired during prenatal development or within the first four weeks of life.[1] Neonatal infections may be contracted by mother to child transmission, in the birth canal during childbirth, or after birth.[2] Neonatal infections may present soon after delivery, or take several weeks to show symptoms. Some neonatal infections such as HIV, hepatitis B, and malaria do not become apparent until much later. Signs and symptoms of infection may include respiratory distress, temperature instability, irritability, poor feeding, failure to thrive, persistent crying and skin rashes.
Risk factors include previous maternal infection, preterm delivery (< 37 weeks gestation) and premature rupture of membranes (breakage of the amniotic sac) which substantially increases the risk of neonatal sepsis by allowing passage for bacteria to enter the womb prior to the birth of the infant. Preterm or low birth weight neonates are more vulnerable to neonatal infection. While preterm neonates are at a particularly high risk, all neonates can develop infection. Maternal screening for intrapartum infections reduce the risk of neonatal infection. Pregnant women may receive intrapartum antibiotic prophylaxis for prevention of neonatal infection.[3]
Infant respiratory distress syndrome is a common complication of neonatal infection, a condition that causes difficulty breathing in preterm neonates. Respiratory distress syndrome can arise following neonatal infection, and this syndrome may have long-term negative consequences. In some instances, neonatal respiratory tract diseases may increase the susceptibility to future respiratory infections and inflammatory responses related to lung disease.[4]
Antibiotics can be effective for neonatal infections, especially when the pathogen is quickly identified. Instead of relying solely on culturing techniques, pathogen identification has improved substantially with advancing technology; however, neonate mortality reduction has not kept pace. In industrialized countries, treatment for neonatal infections takes place in the neonatal intensive care unit (NICU). Neonatal infection can be distressing to the family and it initiates concentrated effort to treat it by clinicians. Research to improve treatment of infections and prophylactic treatment of the mother to avoid infections of the infant is ongoing.[5]
Signs and symptoms
[edit]Signs and symptoms of infection include respiratory distress, temperature instability, irritability, failure to thrive, and skin rashes.[citation needed]
Etiologies
[edit]Early-onset sepsis (EOS), defined as onset of symptoms within 72 hours of life, is generally caused by transmission of pathogens from the female genitourinary system to the fetus. Pathogens can infect the fetus via vertical transmission (direct transmission through the placenta in utero) or infection during delivery as fetus passes through vaginal canal.
Late-onset sepsis (LOS), defined as onset of symptoms after 72 hours of life, is generally caused by transmission of pathogens from the environment after delivery. Infants requiring intravascular catheters and other invasive procedures are at increased risk for developing LOS.[3]
There are many etiologies of neonatal infection, including bacterial, viral and fungal pathogens. The source of infectious bacteria and other pathogens is often the maternal gastrointestinal and genitourinary tract. Many of the maternal infections with these organisms are asymptomatic in the mother. Other maternal infections that may be transmitted to the infant in utero or during birth are bacterial and viral sexually transmitted infections. The infant's ability to resist infection is limited by its immature immune system. In addition, the immune system of the neonate may respond in ways that can create problems that complicate treatment, such as the release of inflammatory chemicals. Congenital defects of the immune system also affect the infants ability to fight off the infection.[6]
Bacteria
[edit]Bacteria found in the maternal gastrointestinal or gastrourinary tracts can commonly lead to neonatal infection. Bacterial infections may present as fetal distress at birth (including signs of tachycardia, temperature instability or difficulty breathing), neonatal sepsis, or neonatal meningitis. Infections that develop during NICU admissions are more commonly coagulase-negative staphylococci, especially in infants with indwelling catheters. Infections that develop one month after the birth of the infant are more likely due to gram-positive bacteria and coagulase positive staphylococci.[7] ...
Group B streptococcus (GBS)
[edit]Group B streptococcus (GBS), also named Streptococcus agalactiae, is a bacteria typically identified as the cause of the majority of early-onset infections in the neonate. GBS is an encapsulated gram-positive cocci that colonizes the gastrointestinal and genital tracts of pregnant women. Maternal infections are usually asymptomatic. This pathogen is vertically transmitted (transmitted directly from the mother's vagina into the infant's amniotic fluid after onset of labor). Due to the high prevalence of GBS, routine screening for the bacteria occurs during pregnancy. If the bacteria is found in the maternal GI / GU tract, mothers will receive IV antibiotic (usually penicillin or ampicillin).[8]
Escherichia coli (E. coli)
[edit]Escherichia coli is an encapsulated gram-negative bacilli that may cause neonatal infections due to its high prevalence in the GI and GU tracts of pregnant patients. With the advances in preventing group B streptococcus infections, β-lactam-resistant Escherichia coli infections have increased in causing neonatal deaths in very low birthweight and premature infants. Common complications of neonatal E.coli infection include neonatal sepsis and neonatal meningitis.[9]
Neisseria gonorrhoeae
[edit]Neisseria gonorrhoeae is a common sexually transmitted infection which may be present in pregnant women at time of delivery. This pathogen is usually acquired during delivery, occurring in 30-40% of cases with known maternal infection. Additionally, untreated maternal gonorrhea may increase the risk of preterm delivery. The most common manifestation of gonococcal infection in a newborn is neonatal conjunctivitis, an infection of the eyes that presents with green-yellow exudate and eyelid swelling. Without treatment, this infection can lead to permanent visual impairment. Treatment of Neisseria gonorrhoeae conjunctivitis consists of a single dose of ceftriaxone (antibiotic). Typically, all neonates (regardless of symptoms or risk factors) receive erythromycin ointment applied to both eyes after delivery[10]
Listeria monocytogenes
[edit]Listeria monocytogenes is a gram-positive bacilli that can cause infection acquired from tainted food and present in the mother. The presence of this pathogen can sometimes be determined by the symptoms that appear as a gastrointestinal illness in the mother. The mother acquires infection from ingesting food that contains animal products such as hot dogs, unpasteurized milk, delicatessen meats, and cheese.[11]
Clostridium tetani
[edit]Clostridium tetani can cause a generalised form of tetanus in the neonate. This usually occurs when the mother has not been vaccinated against tetanus and the baby has not acquired passive immunity. The umbilical cord region is the most susceptible.[12]
Other bacterial pathogens
[edit]Less common bacterial pathogens include Streptococcus pyogenes, Viridans streptococci, Streptococcus pneumoniae, Haemophilus influenzae, and Pseudomonas aeruginosa.[13][citation needed]
Viruses
[edit]Human immunodeficiency virus (HIV)
[edit]Human immunodeficiency virus (HIV) infection can occur during delivery of the neonate, in utero through mother-to-child transmission or postnatally by way of breastfeeding. Most transmission occurs during delivery. Transmission depends on multiple risk factors, usually centered around the viral load of HIV in the mother. Strategies for reducing transmission of HIV include:
- Anti-retroviral therapy during pregnancy, reducing amount of HIV virus in the maternal bloodstream
- Delivery by caesarean section in mothers with plasma viral load > 1000 copies / mL
- Using prophylactic anti-retroviral therapy in the newborn infant, especially in mothers with high viral loads
- Avoiding breast-feeding[14]
Symptoms of HIV in a child will vary depending on the age of presentation. Common symptoms include failure to thrive, recurrent infections such as pneumonia, intermittent diarrhea, swollen lymph nodes and oral thrush. In infants, diagnostic testing for HIV relies of detection of the virus in the bloodstream. For infants born to HIV-infected mothers, diagnostic testing will be performed within days of delivery, at 1–2 months and at 4–6 months of age.[15]
Cytomegalovirus (CMV)
[edit]Cytomegalovirus (CMV) is the most common congenital viral infection, usually transmitted through the placenta during pregnancy. Most neonates with congenital CMV infection will not have any symptoms, but a minority of infected newborns will have symptomatic infection. Common symptoms include rash, microcephaly (small head), low birth weight, jaundice, thrombocytopenia, seizures and retinitis. Long-term complications of congenital CMV infections may include sensorineural hearing loss, developmental delay, and seizures. Due to high prevalence of disease, CMV is not routinely screened in pregnant patients.[16]
Herpes simplex virus (HSV)
[edit]Herpes simplex virus (HSV), which commonly causes cold sores and painful genital blisters can cause congenital infection via direct contact with genital tract lesions during delivery. Neonatal HSV may be classified into three categories based on symptom presentation:
- Localized skin, eye and mouth disease: 35–45% of neonatal HSV infections. Presentation includes clustering vesicular lesions (blister-like) with erythematous (skin redness) base in localized area of skin which can spread to the eye or oropharynx. There is risk of progression to CNS or disseminated disease, so infants should be thoroughly evaluated for progression of symptoms.
- CNS disease: 30% of neonatal HSV infections. HSV spreads into the brain, leading to seizures, lethargy, irritability, poor feeding, temperature instability within the first six weeks of life. Diagnosis of CNS disease can be made with cerebrospinal fluid analysis or electroencephalogram (EEG) showing lateralized periodic discharges. It can be difficult to distinguish between HSV CNS disease and other causes of neonatal meningitis; therefore, it is recommended to start empiric acyclovir in all cases of neonatal meningitis.
- Disseminated disease: 25–30% of neonatal HSV infections. Disease is defined by multi-organ involvement, including liver, lungs CNS, heart, kidney, GI tract, and skin. Neonates with disseminated HSV infection present with nonspecific symptoms of neonatal sepsis. All infants with signs of neonatal sepsis should undergo testing for HSV and empiric antiviral therapy.[17]
Rubella
[edit]Maternal infection with rubella virus during pregnancy can lead to congenital rubella syndrome. The risk of congenital infection is highest during the first trimester (< 12 weeks). Risk of congenital rubella is increased among immigrant women from countries without adequate vaccination programs. Common symptoms include cataracts, hearing impairment, developmental delay and congenital heart disease.[18]
Zika
[edit]Zika virus is an arthropod-borne virus transmitted by mosquitos, and infection during pregnancy can lead to severe congenital abnormalities in a newborn. Congenital infection can lead to fetal growth restriction and CNS abnormalities, including microcephaly, ventriculomegaly and intracranial calcifications.[19]
Hepatitis
[edit]There are five liver specific viruses (hepatitis A, B, C, D, E) that could potentially harm the mother and child. Acute hepatitis A virus or acute hepatitis E virus infection present the greatest risk to maternal and fetal health and increased risk of adverse pregnancy outcomes. Hepatitis B, C and D virus present a risk of mother to child transmission but are dependent on the severity of the underlying disease in the mother. However, hepatitis B virus is the major cause of neonatal infection.[20]
- Hepatitis A is a non-enveloped, single-stranded RNA virus that is spread through the fecal-oral route with the main modes of transmission being close personal contact or ingestion of contaminated food or water. During pregnancy, hepatitis A can cause placental abruption, premature rupture of membranes, and increased rates of preterm labor.[20]
- Hepatitis B is an enveloped, double stranded DNA virus that is spread by exposure to blood, with the main modes of transmission are blood, sexual transmission, or perinatal. During pregnancy, acute hepatitis B infection can result in increased risk of preterm delivery, low birth weight and increased risk of gestational diabetes mellitus. Chronic hepatitis B infection is the largest concern globally. Chronic hepatitis B infection can lead to acute liver failure and increased alanine aminotransferase flares. There is also an increased risk of mother to child transmission and occurs during the delivery of the neonate from an infected mother. Some infected neonates will develop acute hepatitis B and symptomatically will develop abdominal distension, jaundice, clay- colored stools and failure to thrive. However, most infected neonates will be asymptomatic but will chronically have persistent hepatitis B surface antigens in the blood and elevated transaminase levels.[20][21]
- Hepatitis C is an enveloped, single stranded RNA virus that is spread by exposure to blood, with the main modes of transmission are blood, sexual transmission, or perinatal. Chronic infection with hepatitis C virus may influence pregnancy outcomes, such as increased rates of small for gestational age, intrauterine death, low birthweight, and preterm delivery, but no clear association between these adverse outcomes and hepatitis C infection have been observed. There is also an increased risk of mother to child transmission and is largely attributable to events during the birth process.[20]
- Hepatitis D is a single stranded RNA virus that is spread by exposure to blood, with the main modes of transmission are blood, sexual transmission, or perinatal. There is limited research on the effects of hepatitis D infection on fetal or infant outcomes, but the effects are thought to be similar to those with hepatitis B infection.[20]
- Hepatitis E is a non-enveloped, single stranded RNA virus that is spread through the fecal-oral route with the main modes of transmission being close personal contact or ingestion of contaminated food or water. During pregnancy, acute hepatitis E infections result in an increase in adverse pregnancy outcomes such as increased maternal and fetal morbidity and mortality, acute hepatic failure, and associated complications with preterm birth.[20]
Other viral pathogens
[edit]Other viral infections, such as respiratory syncytial virus (RSV), metapneumovirus (hMPV), rhinovirus, parainfluenza (PIV), and human coronavirus in the neonatal period are associated with recurrent wheezing in later childhood.[citation needed]
Fungi
[edit]In very low birth weight infants (VLBWI), systemic fungus infection is a hospital-acquired infection with serious consequences. The pathogens are usually Candida albicans and Candida parapsilosis. A small percentage of fungal infections are caused by Aspergillus, Zygomycetes, Malassezia, and Trichosporon.[22][23] Infection is usually late-onset. Up to 9% of VLBWI with birth weights of <1,000 g develop these fungus infections leading to sepsis or meningitis. As many as one-third of these infants can die. Candidiasis is associated with retinopathy, prematurity and negative neurodevelopmental consequences. Candida can colonize the gastrointestinal tract of low birthweight infants (LBI). This gastrointestinal colonization is often a precursor to a more serious invasive infection. The risk of serious candida infection increases when multiple factors are present. These are: thrombocytopenia, the presence of candidal dermatitis, the use of systemic steroids, birth weights of <1,000 g, presence of a central catheter, postponing enteral feeding, vaginal delivery, and the amount of time broad-spectrum antibiotics were given.[23]
Protozoans
[edit]Infants born with malaria can be infected with a variety of species; Plasmodium vivax, Plasmodium malariae, Plasmodium ovale, and Plasmodium falciparum. In most instances of congenital malaria is caused by P. vivax and P. falciparum. Women living in areas where malaria is prevalent and common are repeatedly exposed to malaria. In response to maternal infection, mothers develop antimalarial antibodies. It is probable that the antibodies present in the mother offers protection for the baby. Bacterial infection can develop with malaria.[22]
Infants that are infected by the protozoan Toxoplasma gondii in utero can be born with chorioretinitis or ocular toxoplasmosis. Globally, it is the most common cause of infections of the back of the eye. (posterior segment). The most common sign is decreased vision in one eye. Other signs and symptoms may appear after the neonatal period and include: chorioretinitis development later in life, intracranial calcification hydrocephalus or central nervous system abnormalities.[24]
Risk factors
[edit]Preterm neonates are at greater risk of infection, including severe complications such as sepsis and meningitis. Preterm neonates usually have ineffective immune systems, due to decreased IgG antibodies and decreased complement activation. Additionally, preterm neonates require longer hospital admissions, including the placement of invasive devices that increase risk of infection.[citation needed]
Maternal risk factors for neonatal infection include:
- Chorioamnionitis - acute inflammation of amniotic fluid and fetal membranes during pregnancy, usually caused by polymicrobial bacterial infection. Signs of infection include maternal fever, vaginal discharge, tender uterus or pain with urination.
- GBS Colonization - group B streptococcus is a bacterial pathogen commonly found in the gastrointestinal and vaginal membranes of healthy women. Presence of this bacteria is usually asymptomatic; therefore, pregnant patients will routinely be screened for presence of GBS prior to delivery.
- Delivery Before 37 Weeks - premature infants require more medical intervention and have less effective immune defenses, so these neonates are at increased risk of infection
- Prolonged Rupture of Membranes (PROM) - the amount of time between the rupture of amniotic membranes and delivery of the neonate is directly correlated with risk of neonatal infection. Prolonged course of labor increases neonatal exposure to bacterial and viral pathogens, increasing chance of infection.[25]
Mechanism
[edit]
Inflammation accompanies infection and is likely to complicate treatment and recovery. Inflammation is linked to reduced growth of the lungs of the premature baby.[26]
Pathogenesis
[edit]The recent identification of the presence of microorganisms in maternal-infant body fluids that were previously thought to be sterile has provided one explanation for the presence of the inflammatory response in both the mother and infant. Sixty-one percent of pregnant women with chorioamnionitis, or inflammation of the amniotic fluid, were found to be infected by microorganisms. Often, more than one pathogen was present. In fifteen percent of pregnant women inflammation was still evident even though there was no evidence of pathogens. This may indicate that there are other causes. A high percentage, 51% to 62%, of pregnant women who had chorioamnionitis also had inflammation of the placenta.[26]
Diagnosis
[edit]Diagnosis of infection is based upon the recovery of the pathogen or pathogens from the typically sterile sites in the mother or the baby. Unfortunately, as many half of pregnant women are asymptomatic with a gonorrhea infection and other sexually transmitted infections.[27][28][29] Samples are obtained from urine, blood or cerebrospinal fluid. Diagnosis of infection can also be aided by the use of more nonspecific tests such as determining the total white blood cell count, cytokine levels and other blood tests and signs.[30]
| Signs of infection | Notes | References |
|---|---|---|
| abnormal complete blood count | looking for signs of infection in the blood: increased white cell count; presence of immature neutrophils |
[31][32] |
| increased C-reactive protein | a chemical in the blood that shows that the baby's immune system is actively reacting to infection |
[31][32][33] |
| accessory muscle use | using the intercostal muscles to assist in breathing |
[32] |
| tachycardia | a heart rate that is faster than normal | [31] |
| bradycardia | a heart rate that is slower than normal | [31] |
| chest recession | [32] | |
| respiratory distress | the baby has trouble breathing | [31][32] |
| nasal flaring | the baby's nostrils expand when it inhales |
[32] |
| expiratory grunt | a sound of effort when the baby exhales | [32][34] |
| apnea | the baby stops breathing | [31][32] |
| rash | [32] | |
| positive urine culture | [31] | |
| positive cerebral spinal fluid | [31] | |
| other positive cultures | from eyes, ear canal, umbilicus axilla anus |
[31] |
| lethargy | the baby seems tired and has slow or no movements | [31][32] |
| hypotonia | the muscles seem flabby and weak | [31][32] |
| hypothermia | [31] | |
| irritability | infant appears uncomfortable and has difficulty being soothed |
[31][32] |
| weak cry | [32] | |
| pneumonia | [31] | |
| poor perfusion | poor circulation | [31][32] |
| hypotension | low blood pressure | [32] |
| acidosis | pH imbalance in the blood | [31][32] |
| diarrhea | water-like, unformed stools | [32] |
| poor feeding | [31] | |
| oxygen requirement | [31] | |
| bulging fontanel | the soft spot on the head is bulging | [32] |
| seizures | [31][32] | |
| fever | [31] | |
| disseminated intravascular coagulation | widespread clotting of blood | [32] |
| kidney failure | kidneys do not function | [32] |
| bacteremia | bacteria cultured from the blood of the newborn |
[31] |
Viral infection
[edit]Symptoms and the isolation of the virus pathogen the upper respiratory tract is diagnostic. Virus identification is specific immunologic methods and PCR. The presence of the virus can be rapidly confirmed by the detection of the virus antigen. The methods and materials used for identifying the RSV virus has a specificity and sensitivity approaching 85% to 95%. Not all studies confirm this sensitivity. Antigen detection has comparatively lower sensitivity rates that approach 65% to 75%.[35]
Protozoan infection
[edit]Congential malaria has its own set of signs:
| Signs of congenital malaria infection | Notes | References |
|---|---|---|
| splenomegaly | enlarged speen | |
| fever | ||
| anemia | ||
| jaundice | ||
| poor feeding | ||
| hepatomegaly | enlarged liver | |
| failure to thrive | ||
| loose stools | ||
| irritability | ||
| hyperbilirubinemia | ||
| central nervous system infection | ||
| splenic rupture | ||
| kidney failure | ||
| blackwater fever | infection with P. falciparum only |
[22] |
Neonatal sepsis
[edit]Neonatal sepsis of the newborn is an infection that has spread through the entire body. The inflammatory response to this systematic infection can be as serious as the infection itself.[26] In infants that weigh under 1500 g, sepsis is the most common cause of death. Three to four percent of infants per 1000 births contract sepsis. The mortality rate from sepsis is near 25%.[36] Infected sepsis in an infant can be identified by culturing the blood and spinal fluid and if suspected, intravenous antibiotics are usually started. Lumbar puncture is controversial because in some cases it has found not to be necessary while concurrently, without it estimates of missing up to one third of infants with meningitis is predicted.[30]
Prevention
[edit]To reduce neonatal infection, screening of pregnant women for HIV, hepatitis B, and syphilis, is available in the UK and the United States.[37][38]
Treatment with a vaginal antibiotic wash prior to birth does not prevent infection with group B streptococcus bacteria (GBS).[31][39] Treatment with vaginal chlorhexidine prior to birth does not prevent neonatal infections.[40]
Because GBS bacteria can colonize the lower reproductive tract of 30% of women, typically pregnant women are tested for this pathogen from 35 to 37 weeks of pregnancy. Before delivery treatment of the mother with antibiotics reduces the rate of neonatal infection.[31] Prevention of the infection of the baby is done by treating the mother with penicillin. Since the adoption of this prophylactic treatment, infant mortality from GBS infection has decreased by 80%.[36]
Mothers with symptomatic genital herpes and who are treated with antiviral prophylaxis are less prone to have an active, symptomatic case at the time of birth and it may be able to reduce the risk of passing on HSV during birth. Cesarean delivery reduces the risk of infection of the infant.[41]
Breastfeeding has been shown to protect the neonate from some infections.[42][43][44][45][46] [excessive citations] Breast milk protects against necrotizing enterocolitis.[47]
Hepatitis A, B, and D are preventable via vaccination. Hepatitis A can be prevented by immunization against HAV, while Hepatitis B and D can both be prevented by immunization against HBV.[20]
The Hepatitis B vaccination is among the first two injections a newborn receives.[48] The other is vitamin K to prevent vitamin K deficiency bleeding.[49] In cases where the pregnant woman is positive for hepatitis B, the baby will receive an additional dose of hepatitis B immunoglobulin in addition to the hepatitis B vaccine to prevent transmission of the disease from mother to baby.[50] Prevention of hepatitis B is crucial as there is no currently no cure.[51]
In general, in an unvaccinated individual, the viral hepatitis family causes liver damage due to a cell-mediated response via cytotoxic lymphocytes.[52] Acute viral hepatitis can lead to jaundice, elevated bilirubin, elevated liver enzymes (aspartate transaminase, alanine transaminase, and alkaline phosphatase), and flu-like symptoms.[52] Importantly, acute neonatal HBV infections progress to chronic Hepatitis B about 90% of the time.[53] For both Hepatitis B and Hepatitis D, the most significant long-term complications are progression to cirrhosis and hepatocellular carcinoma, which carries high morbidity and mortality.[54]
Treatment
[edit]Neonatal infection treatment is typically started before the diagnosis of the cause can be confirmed. Neonatal infection can be prophylactically treated with antibiotics.[55] Maternal treatment with antibiotics is primarily used to protect against group B streptococcus.[30]
Women with a history of genital herpes, can be treated with antiviral drugs to prevent symptomatic lesions and viral shedding that could infect the infant at birth. The antiviral medications used include acyclovir, penciclovir, valacyclovir, and famciclovir. Only very small amounts of the drug can be detected in the fetus. There are no increases in drug-related abnormalities in the infant that could be attributed to acyclovir. Long-term effects of antiviral medications have not been evaluated for their effects after growth and development of the child occurs. Neutropenia can be a complication of acyclovir treatment of neonatal HSV infection, but is usually transient.[41] Treatment with immunoglobulin therapy has not been proven to be effective and is not recommended.[56]
Epidemiology
[edit]Up to 3.3 million newborns die each year and 23.4% of these die of neonatal infection. About half of the deaths caused by sepsis or pneumonia happen in the first week postpartum. In industrialized countries, prophylactic antibiotic treatment of the mothers identified with group B streptococcus, early identification of sepsis in the newborn, and administration of antibiotics to the newborn has reduced mortality.[31] Neonatal herpes in North America is estimated to be from 5 – 80 per 100,000 live births. HSV has a lower prevalence in mothers outside the United States. In the United Kingdom the incidence is much lower and estimated to be 1.6 per 100,000 live births. Approximately 70% to 80% of infected infants are born to mothers with no reported history of HSV infection.[41]
Regions with low neonatal mortality include Europe, the Western Pacific, and the Americas, which have sepsis rates that account for 9.1% to 15.3% of the total neonatal deaths worldwide. This is in contrast with the 22.5 to 27.2% percentage of total deaths in resource-poor countries such as Nigeria, the Democratic Republic of the Congo, India, Pakistan, and China.[31]
In the UK, the proportions of pregnant women who are newly screened positive for hepatitis B, syphilis, and HIV have remained constant since 2010 at about 0.4%, 0.14% and 0.15%, respectively. Estimated prevalence levels among pregnant women for hepatitis B and HIV, including previous diagnoses, were higher at 0.67% and 0.27%. Pregnant women evaluated as susceptible to rubella due to low antibody levels have increased by over 60%, to about 7.2%. However, this increase is probably due to changes in testing methods and evaluation criteria.[57]
In North America, prior to the 1950s, group A β-hemolytic streptococcus (GAS) was the most common pathogen associated with neonatal sepsis prior to the 1960s. In the past twenty years, the most common pathogen causing sepsis is coagulase-negative staphylococci that exist as biofilms associated with infected central venous or arterial catheters.[55] Infections can be fatal and contribute to long-term morbidity and disability among the infants who survive into childhood.[55] Neonatal sepsis effects 128 cases per 1000 live births. Meningitis can occur in the septic infant.[30] Expectant mothers with HSV have a 75% chance of at least one flare-up during their pregnancy.[41] In limited studies it was found that infants in Africa born to mothers with malaria have a 7% of acquiring congenital malaria.[22]
Early-onset infections
[edit]Early onset sepsis can occur in the first week of life. It usually is apparent on the first day after birth. This type of infection is usually acquired before the birth of the infant. Premature rupture of membranes and other obstetrical complications can add to the risk of early-onset sepsis. If the amniotic membrane has been ruptured greater than 18 hours before delivery the infant may be at more risk for this complication. Prematurity, low birth weight, chorioamnionitis, maternal urinary tract infection and/or maternal fever are complications that increase the risk for early-onset sepsis. Early onset sepsis is indicated by serious respiratory symptoms. The infant usually develops pneumonia, hypothermia, or shock. The mortality rate is 30 to 50%.[30]
Late onset infections
[edit]Infections that occur after the first week of life but before the age of 30 days are considered late onset infections. Obstetrical and maternal complications are not typically the cause of these late onset infections; they are usually acquired by the infant in the hospital neonatal intensive care unit. The widespread use of broad-spectrum antibiotics in the nursery intensive care unit can cause a higher prevalence of invasive antibiotic resistant bacteria.[30] Meconium aspiration syndrome has a mortality rate just over 4%. This accounts for 2% for all neonatal deaths.[58]
Research
[edit]The susceptibility to risk of infection and immune deficiencies are active areas of research. Studies regarding the role of viruses in neonatal infections are lacking. Research also continues into the role and protective effect of gut, skin and other human microbiomes and the colonization during the neonatal period.[26][30] The comparison between both resource rich and poor countries makes it difficult to compare the diagnosis success; as industrialized regions are able to confirm the diagnosis and presence of pathogens in the clinical laboratory. Clinical testing may not be available in all settings and clinicians must rely on the signs of infection in the newborn. Research data from Africa and Southeast Asia is scarce.[31]
The result of some research has been the identification of diagnostic tools and procedures that could identify mothers with group B streptococcus infection in resource-poor regions. These procedures would be easy and inexpensive to use. Those mothers who are identified as being infected could then be prophylactly treated prior to the birth of the baby.[31]
Probiotic administration of Lactobacillus species has shown some success.[59]
A GBS vaccine is currently being tested but not currently available. Vaccination is estimated to being able to prevent 4% of GBS infections for preterm births and 60–70% for neonatal GBS infections in the US. The projected benefits of maternal vaccination is the prevention of 899 cases of GBS disease and 35 deaths among infants. The cost savings in the prevention of GBS may be over 43 million dollars. Vaccination may be especially beneficial in low to middle income countries where screening and prophylactic treatment is not possible. Analysts project that GBS vaccination would prevent 30–54% of infant GBS cases. Screening, prophylactic antibiotics and vaccine would prevent 48% of infection.[60]
See also
[edit]References
[edit]- ^ Neil K. Kaneshiro; David Zieve; Isla Ogilvie, eds. (December 4, 2013). "Neonate". U.S. National Library of Medicine. Retrieved January 16, 2016.
- ^ Mary T. Caserta (October 2015). "Overview of Neonatal Infections". Merck Sharp & Dohme Corporation. Retrieved January 16, 2015.
- ^ a b Singh M, Alsaleem M, Gray CP (September 2022). Neonatal Sepsis. StatPearls [Internet]. StatPearls Publishing. PMID 30285373. NBK531478.
- ^ Reuter S, Moser C, Baack M (October 2014). "Respiratory distress in the newborn". Pediatr Rev. 35 (10): 417–28, quiz 429. doi:10.1542/pir.35-10-417. PMC 4533247. PMID 25274969.
- ^ Brenda L Tesini (September 2022). "Antibiotics in Neonates". Merck Sharp & Dohme Corporation. Retrieved February 16, 2023.
- ^ Camacho-Gonzalez A, Spearman PW, Stoll BJ (April 2013). "Neonatal infectious diseases: evaluation of neonatal sepsis". Pediatr Clin North Am. 60 (2): 367–89. doi:10.1016/j.pcl.2012.12.003. PMC 4405627. PMID 23481106.
- ^ Cantey, Joseph B; Edwards, Morven S (2022). "Clinical features, evaluation, and diagnosis of sepsis in term and late preterm neonates" Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. (Accessed on January 31, 2023)
- ^ Santos RP, Tristram D (April 2015). "A practical guide to the diagnosis, treatment, and prevention of neonatal infections". Pediatr Clin North Am. 62 (2): 491–508. doi:10.1016/j.pcl.2014.11.010. PMC 7127476. PMID 25836710.
- ^ Makvana S, Krilov LR (April 2015). "Escherichia coli Infections". Pediatr Rev. 36 (4): 167–70, quiz 171. doi:10.1542/pir.36-4-167. PMID 25834220.
- ^ Speer, Michael E. (2023). "Gonococcal infection in the newborn" Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. (Accessed on February 16, 2023)
- ^ "People at Risk – Pregnant Women and Newborns". Listeria (Listeriosis). Centers for Disease Control and Prevention. 2024.
Pregnant women and their newborns are much more likely to get a Listeria infection, which is called listeriosis.
- ^ "Neonatal Tetanus" (PDF). Vaccine-Preventable Diseases: Surveillance Standards. World Health Organization. September 2018. p. 3.
NT most often occurs through cutting of the umbilical cord using non-sterile techniques or applying non-sterile traditional remedies to the umbilical cord stump, but infection of the umbilical stump is not always evident. Deliveries carried out by persons with unclean hands or on a contaminated surface are also risk factors for maternal and neonatal tetanus (MNT).
- ^ Ershad M, Mostafa A, Dela Cruz M, Vearrier D (2019). "Neonatal Sepsis". Curr Emerg Hosp Med Rep. 7 (3): 83–90. doi:10.1007/s40138-019-00188-z. PMC 7100521. PMID 32226657.
The organisms and pathogens that are most associated with neonatal sepsis differ depending upon country involved. Pathogens range from gram positive and negative bacteria to viruses and fungi, with bacteria being the most frequently identified. The most commonly implicated bacteria include Staphylococcus aureus, coagulase negative staphylococci (CONS), Streptococcus pneumoniae, Streptococcus pyogenes, Escherichia coli, Klebsiella pneumoniae, Pseudomonas aeruginosa, Salmonella typhi, and Group B streptococcus (GBS)
- ^ Hughes, Brenna L; Cu-Uvin, Susan. (2022). "Intrapartum management of pregnant women with HIV and infant prophylaxis in resource-rich settings" Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. (Accessed on February 16, 2023)
- ^ Abbas M, Bakhtyar A, Bazzi R (September 2022). Neonatal HIV. StatPearls [Internet]. StatPearls Publishing. PMID 33351437. NBK565879.
- ^ Demmler-Harrison, Gail J. (2021). "Congenital cytomegalovirus infection: Clinical features and diagnosis" Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. (Accessed on February 5, 2023).
- ^ Demmler-Harrison, Gail J. (2022). "Neonatal herpes simplex virus infection: Clinical features and diagnosis" Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. (Accessed on January 31, 2023)
- ^ Lanzieri, Tatiana; Redd, Susan; Abernathy, Emily; Icenogle, Joseph. (2022). "Chapter 15: Congenital Rubella Syndrome". Centers for Disease Control and Prevention. Accessed on February 16, 2023.
- ^ "Epidemiological update: Outbreaks of Zika virus and complications potentially linked to the Zika virus infection". European Centre for Disease Prevention and Control. 17 December 2015.
- ^ a b c d e f g Terrault NA, Levy MT, Cheung KW, Jourdain G (12 October 2020). "Viral hepatitis and pregnancy". Nature Reviews Gastroenterology & Hepatology. 18 (2): 117–130. doi:10.1038/s41575-020-00361-w. ISSN 1759-5053. PMID 33046891. S2CID 222320257.
- ^ "Neonatal Hepatitis B Virus (HBV) Infection - Pediatrics". Merck Manuals Professional Edition. Retrieved 2022-09-12.
- ^ a b c d Martin R (2015). Fanaroff and Martin's neonatal-perinatal medicine : diseases of the fetus and infant (10th ed.). Elsevier/Saunders. ISBN 978-1-4557-5617-9. OCLC 892338394.
- ^ a b Cloherty J (2012). Manual of neonatal care (7th ed.). Wolters Kluwer Health/Lippincott Williams & Wilkins. ISBN 978-1-60831-777-6. OCLC 780702594.
- ^ Torgerson PR, Mastroiacovo P (2013). "The global burden of congenital toxoplasmosis: a systematic review". Bulletin of the World Health Organization. 91 (7): 501–508. doi:10.2471/BLT.12.111732. ISSN 0042-9686. PMC 3699792. PMID 23825877.
- ^ Cantey, Joseph B; Edwards, Morven S (2022). "Clinical features, evaluation, and diagnosis of sepsis in term and late preterm neonates" Post TW, ed. UpToDate. Waltham, MA: UpToDate Inc. (Accessed on January 31, 2023
- ^ a b c d Pryhuber GS (2015). "Postnatal Infections and Immunology Affecting Chronic Lung Disease of Prematurity". Clinics in Perinatology. 42 (4): 697–718. doi:10.1016/j.clp.2015.08.002. ISSN 0095-5108. PMC 4660246. PMID 26593074.
- ^ Kumar R, Bronze MS (2015). "Pelvic Inflammatory Disease Empiric Therapy". Medscape. Retrieved 23 January 2019.
- ^ Zakher B, Cantor MD AG, Daeges M, Nelson MD H (December 16, 2014). "Review: Screening for Gonorrhea and Chlamydia: A Systematic Review for the U.S. Prevententive Services Task Force". Annals of Internal Medicine. 161 (12): 884–894. CiteSeerX 10.1.1.691.6232. doi:10.7326/M14-1022. PMID 25244000. S2CID 207538182.
- ^ Kenner C (2014). Comprehensive neonatal nursing care (5th ed.). Springer. ISBN 978-0-8261-0975-0. OCLC 861666378. Access provided by the University of Pittsburgh.
- ^ a b c d e f g Fanaroff A (2013). Klaus & Fanaroff's care of the high-risk neonate (6th ed.). Elsevier/Saunders. ISBN 978-1-4160-4001-9. OCLC 811411131.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z aa Santosham M, Chan GJ, Lee AC, Baqui AH, Tan J, Black RE (2013). "Risk of Early-Onset Neonatal Infection with Maternal Infection or Colonization: A Global Systematic Review and Meta-Analysis". PLOS Medicine. 10 (8): e1001502. doi:10.1371/journal.pmed.1001502. ISSN 1549-1676. PMC 3747995. PMID 23976885.
- ^ a b c d e f g h i j k l m n o p q r s t u Sinha S, Miall L, Jardine L (2012). Essential neonatal medicine (5th ed.). Wiley. ISBN 978-0-470-67040-8. OCLC 827207710.
- ^ van de Laar R, van der Ham DP, Oei SG, Willekes C, Weiner CP, Mol BW (2009). "Accuracy of C-reactive protein determination in predicting chorioamnionitis and neonatal infection in pregnant women with premature rupture of membranes: A systematic review". European Journal of Obstetrics & Gynecology and Reproductive Biology. 147 (2): 124–129. doi:10.1016/j.ejogrb.2009.09.017. ISSN 0301-2115. PMID 19819609.
- ^ "Grunting in Neonates - General Practice Notebook". www.gpnotebook.co.uk. (subscription required)
- ^ Mayhall CG (2012). Hospital epidemiology and infection control (4th ed.). Wolters Kluwer Health/Lippincott Williams & Wilkins. ISBN 978-1-60831-300-6. OCLC 774956026.
- ^ a b Florin T (2011). Netter's pediatrics. Elsevier Saunders. ISBN 978-1-4377-1155-4. OCLC 777971566.
- ^ "Infectious diseases in pregnancy screening: programme overview; Detailed guidance". GOV.UK. 1 January 2015. Retrieved 2016-01-07.
- ^ Koumans EH, Rosen J, Dyke MK, Zell E, Phares CR, Taylor A, Loft J, Schrag S (2012-02-01). "Prevention of mother-to-child transmission of infections during pregnancy: implementation of recommended interventions, United States, 2003-2004". American Journal of Obstetrics & Gynecology. 206 (2): 158.e1–158.e11. doi:10.1016/j.ajog.2011.08.027. ISSN 0002-9378. PMC 4707941. PMID 22030318.
- ^ Ohlsson A, Shah VS, Stade BC, Ohlsson A (2014). "Vaginal chlorhexidine during labour to prevent early-onset neonatal group B streptococcal infection". Reviews. 2014 (12): CD003520. doi:10.1002/14651858.CD003520.pub3. PMC 11262555. PMID 25504106.
- ^ Lumbiganon P, Thinkhamrop J, Thinkhamrop B, Tolosa JE (2014-09-14). "Vaginal chlorhexidine during labour for preventing maternal and neonatal infections (excluding Group B Streptococcal and HIV)". The Cochrane Database of Systematic Reviews. 2014 (9): CD004070. doi:10.1002/14651858.CD004070.pub3. ISSN 1469-493X. PMC 7104295. PMID 25218725.
- ^ a b c d Hollier LM, Wendel GD, Hollier LM (2008). "Third trimester antiviral prophylaxis for preventing maternal genital herpes simplex virus (HSV) recurrences and neonatal infection". Reviews (1): CD004946. doi:10.1002/14651858.CD004946.pub2. PMID 18254066.
- ^ Kunz C, Rodriguez-Palmero M, Koletzko B, Jensen R (June 1999). "Nutritional and biochemical properties of human milk, Part I: General aspects, proteins, and carbohydrates". Clinics in Perinatology. 26 (2): 307–33. doi:10.1016/S0095-5108(18)30055-1. PMID 10394490.
- ^ Rodriguez-Palmero M, Koletzko B, Kunz C, Jensen R (June 1999). "Nutritional and biochemical properties of human milk: II. Lipids, micronutrients, and bioactive factors". Clinics in Perinatology. 26 (2): 335–59. doi:10.1016/S0095-5108(18)30056-3. PMID 10394491.
- ^ Hanson LA, Söderström T (1981). "Human milk: Defense against infection". Progress in Clinical and Biological Research. 61: 147–59. PMID 6798576.
- ^ Van de Perre P (July 2003). "Transfer of antibody via mother's milk". Vaccine. 21 (24): 3374–6. doi:10.1016/S0264-410X(03)00336-0. PMID 12850343.
- ^ Jackson KM, Nazar AM (April 2006). "Breastfeeding, the immune response, and long-term health". The Journal of the American Osteopathic Association. 106 (4): 203–7. PMID 16627775.
- ^ Isaacs D (2014). Evidence-based neonatal infections. Wiley Blackwell. ISBN 978-0-470-65460-6. OCLC 852400063.
- ^ "What parents should know about newborn tests and vaccinations | Your Pregnancy Matters | UT Southwestern Medical Center". utswmed.org. Retrieved 2022-09-19.
- ^ Jullien S (2021-09-08). "Vitamin K prophylaxis in newborns". BMC Pediatrics. 21 (Suppl 1): 350. doi:10.1186/s12887-021-02701-4. ISSN 1471-2431. PMC 8424792. PMID 34496783.
- ^ Eke AC, Eleje GU, Eke UA, Xia Y, Liu J (2017-02-11). "Hepatitis B immunoglobulin during pregnancy for prevention of mother-to-child transmission of hepatitis B virus". The Cochrane Database of Systematic Reviews. 2017 (2): CD008545. doi:10.1002/14651858.CD008545.pub2. ISSN 1469-493X. PMC 6464495. PMID 28188612.
- ^ Suk-Fong Lok A (2018-11-15). "Hepatitis B Treatment: What We Know Now and What Remains to Be Researched". Hepatology Communications. 3 (1): 8–19. doi:10.1002/hep4.1281. ISSN 2471-254X. PMC 6312657. PMID 30619990.
- ^ a b Bertoletti A, Ferrari C (April 2016). "Adaptive immunity in HBV infection". Journal of Hepatology. 64 (1 Suppl): S71–S83. doi:10.1016/j.jhep.2016.01.026. ISSN 1600-0641. PMID 27084039.
- ^ Zhang HW, Yin JH, Li YT, Li CZ, Ren H, Gu CY, Wu HY, Liang XS, Zhang P, Zhao JF, Tan XJ, Lu W, Schaefer S, Cao GW (December 2008). "Risk factors for acute hepatitis B and its progression to chronic hepatitis in Shanghai, China". Gut. 57 (12): 1713–1720. doi:10.1136/gut.2008.157149. ISSN 0017-5749. PMC 2582333. PMID 18755887.
- ^ Yang DH, Wang WP, Zhang Q, Pan HY, Huang YC, Zhang JJ (2021-05-07). "Hepatocellular carcinoma progression in hepatitis B virus-related cirrhosis patients receiving nucleoside (acid) analogs therapy: A retrospective cross-sectional study". World Journal of Gastroenterology. 27 (17): 2025–2038. doi:10.3748/wjg.v27.i17.2025. ISSN 1007-9327. PMC 8108039. PMID 34007137.
- ^ a b c MacDonald M (2015). Avery's neonatology : pathophysiology and management of the newborn (7th ed.). Wolters Kluwer. ISBN 978-1-4511-9268-1. OCLC 922715498.
- ^ Ohlsson A, Lacy JB (29 January 2020). "Intravenous immunoglobulin for suspected or proven infection in neonates". The Cochrane Database of Systematic Reviews. 1 (1): CD001239. doi:10.1002/14651858.CD001239.pub6. ISSN 1469-493X. PMC 6988993. PMID 31995649.
- ^ Infection reports; HIV – STIs Antenatal screening for infectious diseases in England: summary report for 2014 (PDF). Infection reports Volume 9 Number 43 Published on: 4 December 2015 HIV – STIs Antenatal screening for infectious diseases in England: summary report for 2014 (Report). Vol. 9. Public Health England. 4 December 2015. Retrieved 8 January 2016.
- ^ {{cite journal |last1=Siriwachirachai |first1=Thitiporn |last2=Sangkomkamhang |first2=Ussanee S |last3=Lumbiganon |first3=Pisake |last4=Laopaiboon |first4=Malinee |last5=Siriwachirachai |first5=Thitiporn |year=2014 |title=Antibiotics for meconium-stained amniotic fluid in labour for preventing maternal and neonatal infections |journal=Reviews |volume=2014 |issue=11 |pages=CD007772 |doi=10.1002/14651858.CD007772.pub3 |pmc=6823264 |pmid=25374369 }
- ^ Baucells B, Mercadal Hally M, Álvarez Sánchez A, Figueras Aloy J (2015). "Asociaciones de probióticos para la prevención de la enterocolitis necrosante y la reducción de la sepsis tardía y la mortalidad neonatal en recién nacidos pretérmino de menos de 1.500g: una revisión sistemática". Anales de Pediatría. 85 (5): 247–255. doi:10.1016/j.anpedi.2015.07.038. ISSN 1695-4033. PMID 26611880.
- ^ Cortese F, Scicchitano P, Gesualdo M, Filaninno A, De Giorgi E, Schettini F, Laforgia N, Ciccone MM (2015). "Early and Late Infections in Newborns: Where Do We Stand? A Review". Pediatrics & Neonatology. 57 (4): 265–273. doi:10.1016/j.pedneo.2015.09.007. hdl:11586/219777. ISSN 1875-9572. PMID 26750406.
Further reading
[edit]- Jenster M, Bonifacio SL, Ruel T, Rogers EE, Tam EW, Partridge JC, Barkovich AJ, Ferriero DM, Glass HC (2014-07-01). "Maternal or neonatal infection: association with neonatal encephalopathy outcomes". Pediatric Research. 76 (1): 93–99. doi:10.1038/pr.2014.47. ISSN 0031-3998. PMC 4062582. PMID 24713817.
- "Antibiotics for the prevention and treatment of early-onset neonatal infection". National Guideline Clearinghouse. Archived from the original on 2016-01-06. Retrieved 2016-01-15.
External links
[edit]- "Newborn death and illness". World Health Organization. Retrieved 2016-01-15.
